Amniocentesis
Updated: 2022-10-07
Overview
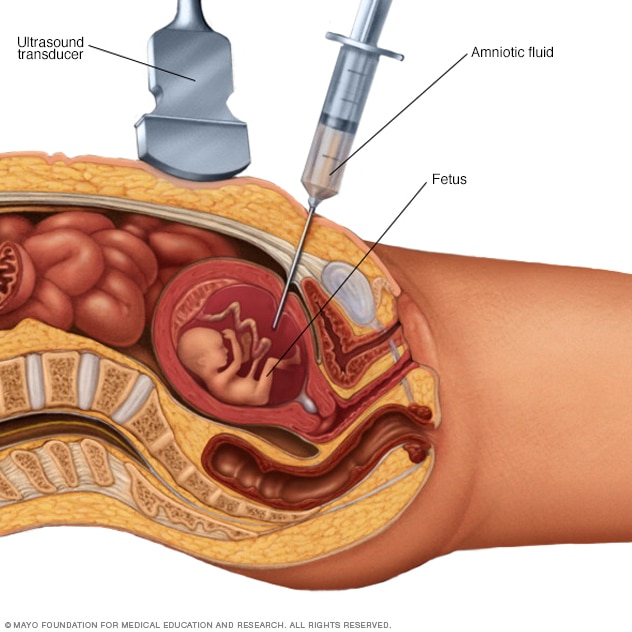
Amniocentesis
Amniocentesis is a test done during pregnancy. During amniocentesis, an ultrasound wand (transducer) is used to show a baby's position in the uterus on a monitor. A sample of amniotic fluid, which contains fetal cells and chemicals produced by the baby, is then taken for testing.
Amniocentesis is done to remove amniotic fluid and cells from the uterus for testing or treatment. Amniotic fluid surrounds and protects a baby during pregnancy.
Amniocentesis can provide useful information about a baby's health. But it's important to know the risks of amniocentesis — and be prepared for the results.
Why it's done
Amniocentesis can be done for a number of reasons:
- Genetic testing. Genetic amniocentesis involves taking a sample of amniotic fluid and testing the DNA from the cells for diagnosis of certain conditions, such as Down syndrome. This might follow another screening test that showed a high risk of the condition.
- Diagnosis of fetal infection. Occasionally, amniocentesis is used to look for infection or other illness in the baby.
- Treatment. Amniocentesis might be done to drain amniotic fluid from the uterus if too much has built up — a condition called polyhydramnios.
- Fetal lung testing. If delivery is planned sooner than 39 weeks, amniotic fluid might be tested to help find out whether a baby's lungs are mature enough for birth. This is rarely done.
Genetic amniocentesis
Genetic amniocentesis can provide information about the baby's genes. Generally, genetic amniocentesis is offered when the test results might affect how to manage the pregnancy.
Genetic amniocentesis is usually done between weeks 14 and 20 of pregnancy. Amniocentesis done before week 14 of pregnancy might lead to more complications.
Reasons to consider genetic amniocentesis include:
- Having positive results from a prenatal screening test. If the results of a screening test — such as the first-trimester screen or prenatal cell-free DNA screening — show high risk or are worrisome, amniocentesis might confirm or rule out a diagnosis.
- Having an earlier pregnancy affected by a genetic condition. A health care provider might suggest amniocentesis to look for that condition.
- Being 35 or older. Babies born to people 35 and older have a higher risk of chromosomal conditions, such as Down syndrome. A health care provider might suggest amniocentesis to rule out these conditions if prenatal cell-free DNA screening is positive.
- Having a family history of a genetic condition, or if the parents are carriers of a genetic condition. Besides identifying Down syndrome, amniocentesis can be used to diagnose other genetic conditions, such as cystic fibrosis.
- Having unusual ultrasound findings. A health care provider might recommend amniocentesis to diagnose or rule out genetic conditions associated with unusual ultrasound findings.
Risks
Amniocentesis carries risks, which occur in approximately 1 in 900 tests. They include:
- Leaking amniotic fluid. Rarely, amniotic fluid leaks through the vagina after amniocentesis. In most cases, the amount of fluid lost is small and stops within one week with no effect on the pregnancy.
- Miscarriage. Second-trimester amniocentesis carries a slight risk of miscarriage — about 0.1% to 0.3% when done by a skilled person using ultrasound. Research suggests that the risk of pregnancy loss is higher for amniocentesis done before 15 weeks of pregnancy.
- Needle injury. During amniocentesis, the baby might move an arm or leg into the path of the needle. Serious needle injuries are rare.
- Rh sensitization. Rarely, amniocentesis might cause the baby's blood cells to enter the pregnant person's bloodstream. Those with Rh negative blood who haven't developed antibodies to Rh positive blood are given an injection of a blood product, Rh immune globulin, after amniocentesis. This prevents the body from making Rh antibodies that can cross the placenta and damage the baby's red blood cells.
- Infection. Very rarely, amniocentesis might trigger a uterine infection.
- Infection transmission. Someone who has an infection — such as hepatitis C, toxoplasmosis or HIV/AIDS — might transfer it to the baby during amniocentesis.
Remember, genetic amniocentesis is usually offered to pregnant people for whom the test results might greatly affect how they manage the pregnancy. The decision to have genetic amniocentesis is yours. Your health care provider or genetic counselor can give you information to help you decide.
How you prepare
Your health care provider will explain the procedure and ask you to sign a consent form. Consider asking someone to accompany you to the appointment for emotional support or to drive you home afterward.
What you can expect
Amniocentesis is usually done in an outpatient obstetric center or a health care provider's office.
During the procedure
First, a health care provider will use ultrasound to pinpoint where the baby is in the uterus. You'll lie on your back on an exam table with your belly showing. Your health care provider will apply a gel to your belly and then use a small device known as an ultrasound transducer to show your baby's position on a monitor.
Next, your health care provider will clean your abdomen. A numbing medication generally isn't used. Most people report only mild soreness during the procedure.
Guided by ultrasound, your health care provider will insert a thin, hollow needle through your stomach wall and into the uterus. A small amount of amniotic fluid is drawn into a syringe. The needle is then removed.
You need to lie still while the needle is put in and the amniotic fluid is taken out. You might feel a sting when the needle enters your skin. You might feel cramping when the needle enters your uterus.
After the procedure
After amniocentesis, your health care provider will continue using the ultrasound to monitor your baby's heart rate. You might have cramping or mild pelvic pain after an amniocentesis.
You can return to your regular activities after the test.
The sample of amniotic fluid will be looked at in a lab. Some results might be available within a few days. Other results might take several weeks.
Contact your health care provider if you have:
- Bleeding or loss of amniotic fluid through the vagina
- Severe uterine cramping that lasts more than a few hours
- Fever
- Redness where the needle was inserted
- Fetal activity that is different than usual or no fetal movement
Results
Your health care provider or a genetic counselor will help you understand your amniocentesis results.
For genetic amniocentesis, test results can rule out or diagnose some genetic conditions, such as Down syndrome. Amniocentesis can't identify all genetic conditions and birth defects.
If amniocentesis suggests that your baby has a genetic or chromosomal condition that can't be treated, you might face hard decisions. Seek support from your health care team and your loved ones.